Cory
Simpson
MD
PhD

Simpson Lab
UW Medicine at South Lake Union
850 Republican St.
Brotman D254
Box 358050
Seattle, WA 98109
Appointments
UW Medical Center – Roosevelt Dermatology Center
206.598.4067
Roos Schedule Online
Biography
Dr. Cory Simpson is a board-certified dermatologist at UW Medical Center's Roosevelt Dermatology Clinic and an Assistant Professor and Researcher in the Department of Dermatology at the University of Washington. A native of Granite City, Illinois, Dr. Simpson received his MD and PhD in Cell Biology from Northwestern University in Chicago, with his doctoral thesis focused on the role of desmosomal cadherins in epidermal differentiation and skin disease. After his residency in dermatology at the University of Pennsylvania, Dr. Simpson spent several years as a Clinical Instructor at Penn’s Perelman School of Medicine in Philadelphia. There, he built a subspecialty clinic focused on patients with inherited and autoimmune bullous disorders, which continues to be his focus at UW. Dr. Simpson’s clinical expertise includes skin blistering diseases such as pemphigus and pemphigoid as well as genetic skin barrier disorders such as ichthyoses, Darier disease, and Hailey-Hailey disease.
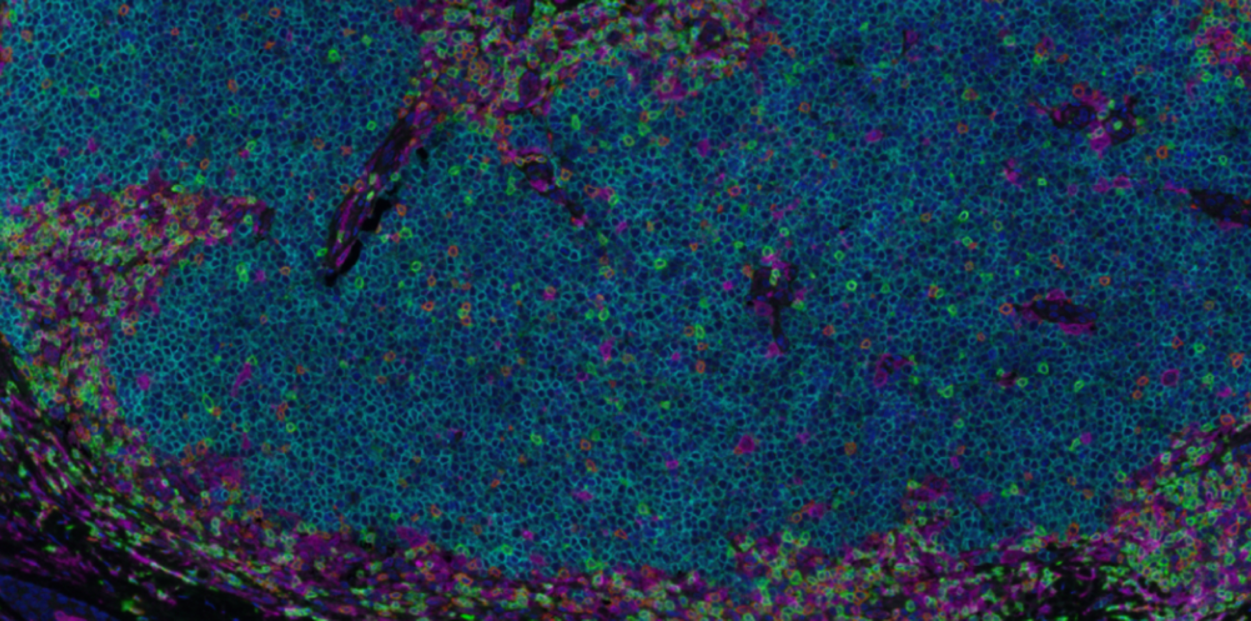
Dr. Simpson launched a research laboratory at the University of Washington in 2021 to study epidermal differentiation and how it is compromised in dermatologic disease. The Simpson Lab focuses on the role of autophagy and organelle degradation in human keratinocytes and how these cellular pathways drive maturation and homeostasis of the epidermal tissue. Using an organotypic model of human skin coupled with advanced microscopy, his lab can visualize the live tissue at the level of single organelles to better understand how the epidermis forms and how disease-associated mutations disrupt the tissue. Ultimately, the Simpson Lab aims to identify novel treatment strategies to promote epidermal tissue regeneration after skin injuries and to restore skin barrier function in inherited and currently incurable dermatologic diseases.
Dr. Simpson’s research has been supported by the National Institutes of Health (NIH), the National Institute of Arthritis and Musculoskeletal and Skin Diseases (NIAMS), the Dermatology Foundation, the American Skin Association, the National Psoriasis Foundation, and the Foundation for Ichthyosis and Related Skin Types (FIRST).
social media
Education & Training
Post-doctoral Fellowship in Cutaneous Biology, Dept. of Physiology, University of Pennsylvania, Perelman School of Medicine, Philadelphia, PA (2016-2021)
Residency in Dermatology, Hospital of the University of Pennsylvania, Philadelphia, PA (2013-2016)
Internship in Internal Medicine, University of Chicago, NorthShore University Health System, Evanston, IL (2012-2013)
PhD, Cell Biology, Northwestern University, Chicago, IL (2005-2010)
MD, Medical Scientist Training Program, Northwestern University, Chicago, IL (2003-2012)
BA in Biology, Minor in Spanish (Summa Cum Laude), Washington University, St. Louis, MO (1999-2003)
Honors
Young Physician-Scientist Award, American Society for Clinical Investigation (2024)
Emerging Leader, Dept. of Medicine, University of Washington (2023)
Outstanding Research Mentor Award, University of Washington School of Medicine (2022)
Patient Care Hero Award for Clinical Volunteerism, American Academy of Dermatology (2019)
Presidential Citation for Teledermatology Outreach, American Academy of Dermatology (2019)
World Congress of Dermatology Scholarship, American Academy of Dermatology (2019)
Mentoring Grant, Diversity Mentorship Program, American Academy of Dermatology (2019)
Research Interests
Dr. Simpson’s research focuses on the skin, which serves as a protective shield between the human body and its environment. The Simpson Lab uses advanced microscopy, gene editing, and organoid epidermis to understand the biology of skin cells called keratinocytes. The goal of their research program is to determine the mechanisms by which keratinocytes regenerate skin tissue and how this process is compromised in dermatologic diseases. Dr. Simpson's research group also models rare genetic skin blistering and cornification disorders in the lab to help find novel treatments for patients.
Clinical Interests
Dr. Simpson’s clinical expertise includes autoimmune blistering diseases such as pemphigus and pemphigoid, genetic blistering diseases like Darier and Hailey-Hailey disease, as well as inherited skin barrier disorders called ichthyoses.
Publications
Selected Publications
Zaver SA, Sarkar MK, Egolf S, Zou J, Tiwaa A, Capell BC, Gudjonsson JE, Simpson CL. Targeting SERCA2 in organotypic epidermis reveals MEK inhibition as a therapeutic strategy for Darier disease. JCI Insight. 2023 Sep 22;8(18). doi: 10.1172/jci.insight.170739. PubMed PMID: 37561594
Zaver SA, Johnson CJ, Berndt A, Simpson CL. Live Imaging with Genetically Encoded Physiologic Sensors and Optogenetic Tools. J Invest Dermatol. 2023 Mar;143(3):353-361.e4. doi: 10.1016/j.jid.2022.12.002
Egolf S, Zou J, Anderson A, Simpson CL, Aubert Y, Prouty S, Ge K, Seykora JT, Capell BC. MLL4 mediates differentiation and tumor suppression through ferroptosis. Sci Adv. 2021 Dec 10;7(50):eabj9141. doi: 10.1126/sciadv.abj9141. Epub 2021 Dec 10. PubMed PMID: 34890228; PubMed Central PMCID: PMC8664260
Simpson CL, Tokito MK, Uppala R, Sarkar MK, Gudjonsson JE, Holzbaur EL. NIX initiates mitochondrial fragmentation via DRP1 to drive epidermal differentiation. Cell Reports. Feb 2; 34(5): 108689. PMID: 33535046
Moore AS, Coscia SM, Simpson CL, Ortega FE, Wait EC, Heddleston JM, Nirschl JJ, Obara CJ, Guedes-Dias P, Boecker CA, Chew T-L, Theriot JA, Lippincott-Schwartz J, Holzbaur EL. Actin cables and comet tails organize mitochondrial networks in mitosis. Nature. 2021 Mar; 591(7851): 659-664. PMID: 33658713
Tamazian S, Simpson CL: Autoimmune bullous disease in skin of color: A case series. JAAD Case Rep, 2020. 6(11):1173-8. PMID: 33145386
Wang LL, Moshiri AS, Novoa R, Simpson CL, Takeshita J, Payne AS, Chu EY (2020): Comparison of C3d immunohistochemical staining to ELISA and immunofluorescence for diagnosis of bullous pemphigoid. J Amer Acad of Dermatol, 2020. 83(1):172-8. PMID: 32068042
Holmes AN, Chansky PB, Simpson CL: Teledermatology consultation can optimize treatment of cutaneous disease by non-dermatologists in under-resourced clinics. Telemed J E Health, 2020. 26(10):1284-90. PMID: 31800369